Bearded Dragon Yellow Fungus – Does Your Dragon Have It
Finding something yellow and crusty on your bearded dragon’s scales sends most owners straight to the worst corner of the internet. Yellow fungus disease is serious. In the wrong circumstances it is life-threateningly serious.
It is also one of the most misidentified conditions in bearded dragon keeping. Thermal burns, stuck shed, and normal colour variation all get mistaken for it regularly. The opposite error happens too: real early yellow fungus gets dismissed as a shedding problem because it looks nothing like the dramatic photos in most articles.
The deciding factor in how this disease plays out is almost always timing. An owner who acts on the first signs has a meaningfully different outcome than one who watches and waits for two weeks to see if it clears on its own.
What Bearded Dragon Yellow Fungus Actually Is
Yellow fungus disease is a fast-progressing fungal infection caused by Nannizziopsis guarroi that attacks skin, tissue, bone, and eventually internal organs. It is not the same as a surface yeast infection or a harmless colour change. It is a primary pathogen that actively invades healthy tissue rather than waiting for a compromised host.
The abbreviation YFD and the term CANV both refer to the same disease. CANV is a holdover from older taxonomy. The original classification, Chrysosporium anamorph of Nannizziopsis vriesii, was revised after molecular testing identified the bearded-dragon-specific strain. Your vet may use either name.
Most fungal infections exploit a weakened immune system. This one does not require one. Poor husbandry, stress, and cohabitation make infection far more likely, but no dragon is immune simply because it is well cared for.
The name CANV is a holdover from older taxonomy referring to Chrysosporium anamorph of Nannizziopsis vriesii, the original classification before molecular testing identified the bearded-dragon-specific strain. Your vet may use either name. Both refer to the same clinical picture. What matters more than the name is the biology: this fungus does not stay on the surface. It moves inward, through skin and tissue, and eventually reaches bone and internal organs if unchecked.
What Early Yellow Fungus Actually Looks Like
This is where most articles fail. Describing YFD as “yellow patches on the skin” tells an owner almost nothing useful about what they are actually looking for in early presentation. By the time the patches are dramatically and obviously yellow, the infection has typically been running for several weeks.
What to actually look for: a small cluster of scales, often no larger than a thumbnail, that appear slightly duller and rougher than the surrounding skin. The texture is the first tell, before the colour becomes alarming. The affected area feels raised at the edges under a fingertip, and the scales do not peel cleanly when the dragon sheds.
Healthy shed skin comes away in sheets or sections and reveals fresh, correct-coloured scales underneath. An early YFD lesion leaves behind a roughened, discoloured surface that persists or worsens after every shed cycle.
The colour at this stage is often amber, pale golden, or matte beige rather than the vivid orange-yellow shown in clinical photographs. If you are waiting for “obviously yellow,” you are already looking at a mid-stage presentation on a dragon that has had the infection for weeks.
The Early Signs
An increase in shedding frequency is one of the earliest observable signs, and it appears in almost no consumer-facing article on this topic. A dragon cycling through sheds faster than usual, looking opaque again almost immediately after finishing one, may be mounting a skin-level immune response to a superficial infection.
A shedding storm on its own does not confirm YFD, and it has other causes, but combined with any roughened or discoloured patch it belongs in a vet call today rather than a forum post next week. A dragon cycling through unusually rapid sheds for no obvious reason is worth monitoring closely regardless.
What It Gets Mistaken For

Thermal burns look strikingly similar to early YFD. Both produce yellow, orange, and brown discolouration with damaged scale texture. The key difference is location and history.
Burns appear on surfaces directly beneath a malfunctioning or improperly positioned heat source: the top of the head, the dorsal surface of the back, the neck area. YFD appears randomly, with no relationship to heat source placement, and commonly starts on the limbs, flanks, or tail.
A recent history of abnormal basking temperatures or thermostat failure points toward a burn. A growing patch in a random location with no identifiable heat event points toward something else. Knowing what an actual thermal burn looks like in early presentation makes this call much easier to make at home.
Stuck shed across multiple cycles leaves thickened, discoloured patches that can read as yellow or brown. The reliable test is a 15-minute warm soak followed by gentle shed assistance. If healthy, correctly-coloured scales emerge underneath, it was retained shed. If the patch remains, or the tissue underneath looks unhealthy, the situation changes entirely. Retained shed that does not lift cleanly after a warm assisted soak is not a shed problem.
Normal pigmentation variation trips up owners who are new to their dragon’s specific colouring, particularly in citrus and yellow morphs. A patch completely static for several months, same size, same texture, no change in appetite or behaviour, is almost certainly not YFD.
The disease does not stay the same. Anything growing, spreading, or changing texture over a two-week observation period needs a vet assessment regardless of what else it might be. The same logic applies to tail darkening, where a dark tail assessment follows the same principles and carries equally high stakes.
When to Call the Vet
Every article on this topic says “see a vet immediately” without giving owners enough detail to calibrate what immediately actually means in their situation. These signs require a same-day call, not a wait-and-see approach:
- The patch is visibly growing between observations a few days apart
- Multiple separate patches have appeared in different locations on the body
- The tissue under the discolouration looks soft, sunken, or is weeping any fluid
- The dragon has reduced appetite alongside any skin abnormality
- The patch persists with unchanged or worsening texture after a full assisted shed
A single static patch on a dragon eating normally and behaving well still warrants a professional assessment, but booking within the week rather than the same day is a reasonable call if none of the above apply. The moment any of those escalation signs appear, that changes.
Not every general practice vet is experienced with reptile skin disease, so if you do not already have an exotic specialist, the ARAV vet directory is the fastest way to find a qualified reptile vet near you.
Your Vet Needs a Biopsy to Confirm It
A biopsy is the only method that confirms YFD. The sample is taken under brief anaesthesia, examined microscopically, and submitted for PCR testing and culture to identify the specific organism involved. Bloodwork assesses internal organ function and the degree of systemic involvement. X-rays may follow if there is any concern about bone penetration, which develops as the disease advances through deeper tissue layers.
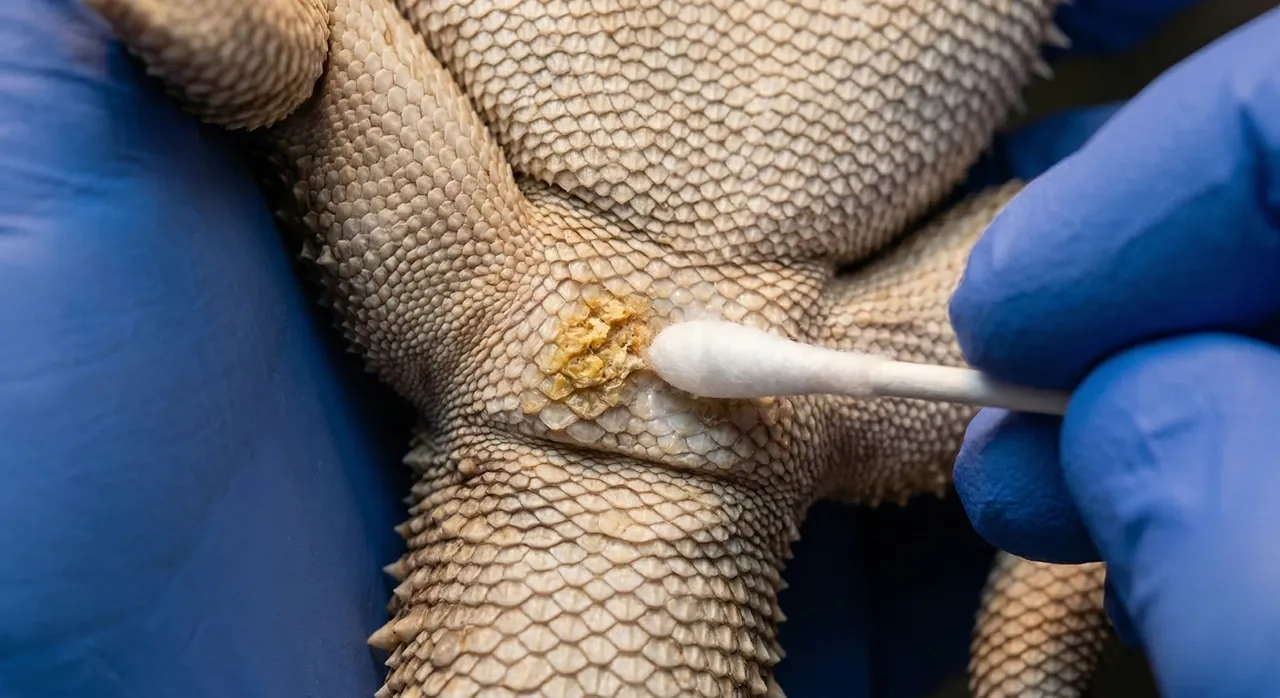
Confirmed treatment centres on oral voriconazole, an antifungal that has shown more promise than older combination protocols using itraconazole or terbinafine. Treatment is not a two-week course. It typically runs for months, requires repeated bloodwork to monitor liver function, and the cost adds up quickly. Topical povidone iodine applied directly to the lesion once or twice daily runs alongside oral medication rather than replacing it.
Where necrotic tissue is present, debridement may be recommended. This is the removal of dead tissue that the fungus actively feeds on, because systemic drugs cannot penetrate tissue that has lost its blood supply. Your vet will assess whether home debridement is appropriate for your specific situation and demonstrate the technique before you attempt it. Not every case warrants it.
The Honest Prognosis
Most articles state flatly that YFD is always fatal, which causes some owners to give up before treatment has started. Others soften the reality so much that the urgency disappears entirely.
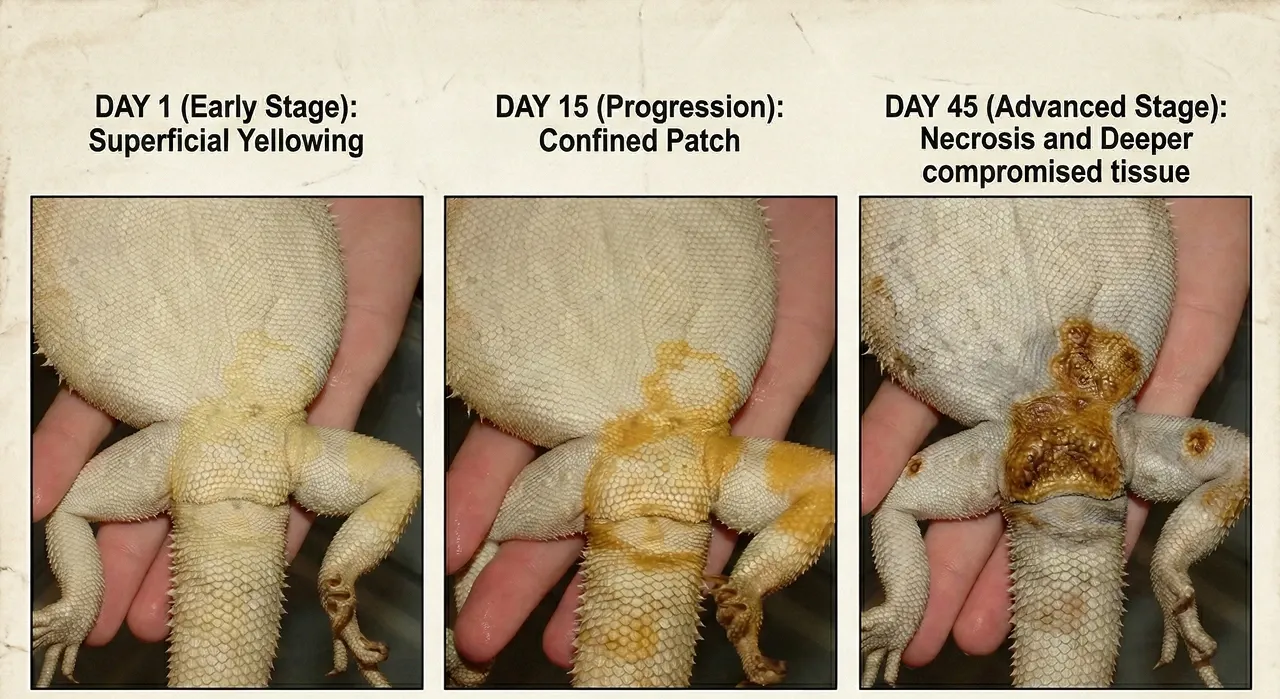
A single superficial lesion caught early, no internal involvement, dragon still eating and active, treated aggressively with voriconazole and consistent topical care: this scenario gives a meaningful chance at extended remission. Remission is the correct word. The infection cannot be fully and reliably cleared with current treatment options, but it can be pushed back far enough that the dragon lives well beyond diagnosis. Some dragons treated at this stage have survived two years and beyond.
Internal involvement, multiple spreading lesions, or significant tissue necrosis carries a far worse outlook. The majority of documented cases with systemic disease result in euthanasia within six months of diagnosis. The difference between these two outcomes is almost entirely determined by how quickly the owner acted on the first sign they noticed something was wrong.
In practice, remission looks like this: the lesion stops growing, no new patches appear, and the affected area firms up rather than continuing to soften or weep. That is the benchmark to measure progress against during treatment.
Strip the Enclosure Immediately
If YFD is confirmed or strongly suspected, treat the enclosure as a contaminated environment from that moment. CANV spreads through direct contact and through the air. The substrate, hides, decor, and enclosure walls all carry infectious load.
Move the dragon to a hospital setup: paper towel substrate, minimal hard plastic decor, wiped down daily with F10SC veterinary disinfectant at a 1:250 dilution in water, or a 1:10 bleach solution rinsed thoroughly and dried completely after contact. Strip the original enclosure completely.
Wooden hides, cork bark, fabric hammocks, and live plants should all be discarded rather than cleaned. Adequate disinfection of porous materials is not reliably achievable. Hard surfaces can be scrubbed, rinsed thoroughly, and dried completely before any reuse.
Symptoms, Causes and Actions at a Glance
| What You See | Dragon’s Behaviour | Most Likely Cause | Action |
|---|---|---|---|
| Yellow or tan patch, no change over months | Eating normally, active | Normal pigmentation or old burn scar | Monitor. Vet check if uncertain. |
| Rough, dull scales after a shed | Eating normally | Stuck shed or early YFD | Assist shed with warm soak. Vet check if patch remains. |
| Patch under basking spot, heat event history | Any | Thermal burn | Vet assessment. Do not assume YFD without biopsy. |
| Growing patch, raised texture, random location | Any | Possible YFD | Vet call today. |
| Multiple patches in different body locations | Reduced appetite | Probable YFD with spread | Same-day vet appointment. |
| Sunken, soft, or weeping tissue | Lethargic, not eating | Advanced YFD or bacterial infection | Emergency vet visit. |
| Abnormally frequent shedding plus any skin change | Any | Early immune response, possible YFD | Vet call. Do not wait for visible lesion to develop. |
Frequently Asked Questions
Is Bearded Dragon Yellow Fungus Contagious to Humans
CANV is not recognised as a zoonotic disease, meaning healthy humans are not at risk from contact with an infected dragon. There are rare documented cases of infection in severely immunocompromised individuals, but these are not considered a realistic risk for healthy owners. Wearing gloves during treatment application is still good practice because you are handling an open infection, not because personal transmission is a real concern.
Can Yellow Fungus Go Away on Its Own
No. CANV is a progressive primary pathogen that does not resolve without treatment. Without intervention the infection spreads inward, and eventually reaches deeper tissue and internal organs. Early-stage remission is achievable with aggressive treatment, but spontaneous resolution does not occur.
How Fast Does Yellow Fungus Spread
There is no reliable average. In a well-nourished dragon under good husbandry, a superficial lesion can hold relatively stable for a few weeks. In a stressed or immunocompromised animal, the same lesion can visibly expand within days. Assuming you have time because the patch looks small is one of the most common mistakes owners make with this disease.
Can I Treat Yellow Fungus at Home
Topical chlorhexidine or povidone iodine can be used as a holding measure while you wait for a vet appointment, but home treatment alone is not sufficient to manage YFD. Oral voriconazole is a prescription medication that requires a veterinary diagnosis to obtain. Treating the surface of an infection that is already progressing internally produces no meaningful result without the systemic component.
What Does Yellow Fungus Smell Like
Advanced lesions with significant necrosis can produce a faint but distinctly unpleasant odour from the dying tissue. Most owners do not notice a smell in the early stages. If you detect an unusual odour near your dragon’s skin during handling, particularly near any discoloured area, that is a strong prompt to book a vet appointment the same day rather than continuing to observe.
What to Do Right Now
Start by examining your dragon in natural light and looking at the texture of any discoloured area before you focus on the colour. Run a fingertip gently across it. If it feels raised, rough, or different from the surrounding scales in any way, photograph it today and photograph it again in three days. Growth between those two photographs answers a lot of questions without requiring a vet opinion.
If the patch is new, appeared with no heat event history, and sits in a random location rather than directly under the basking zone, book a vet assessment rather than treating it as a burn. If the dragon’s appetite has changed at all alongside any skin abnormality, do not wait for the patch to worsen. Call today.
Prevention comes down to three things you already control. A dragon eating a correct diet for its age has a substantially better immune response than one on an inadequate supplement routine.
The enclosure conditions that suppress immune function, sustained temperatures below optimal, high humidity, and chronic stress, are the same conditions that make it harder for a dragon to resist a primary pathogen even in a clean setup. Hygiene, correct temperatures, and keeping your dragon housed alone are the three things within your control.

Written by
Sarah ArdleySarah has kept bearded dragons for over ten years. She founded Beardie Husbandry after discovering that most mainstream care advice — including what she followed with her first dragon — was doing more harm than good. Every article on this site is grounded in veterinary research and real keeper experience.







