What Causes MBD in Bearded Dragons and Can You Reverse It
Bearded dragons that start dragging their hindlegs, trembling when they try to lift their own weight, or showing a jaw that feels softer than it should are sending a clear signal. MBD in bearded dragons is one of the most common health problems keepers encounter, and it almost always traces back to a husbandry gap that has been running silently for months.
Most cases are preventable. A good number are fully recoverable if caught early. The ones that cause permanent damage are usually the ones where the signs were present for a long time but were misread as something else: lethargy from temperature, appetite loss from stress, slow movement from the onset of brumation. Each one bought more time for the disease to progress.
What Actually Causes MBD in Bearded Dragons
Three things have to work together for a dragon to build and maintain healthy bone: dietary calcium, vitamin D3, and UVB light. D3 is the central piece. Without it, calcium cannot be absorbed from the gut regardless of how much you dust onto feeders, because the intestinal pathway that moves calcium into the bloodstream depends on D3 to function.
In captivity, the primary way a dragon produces D3 is by absorbing UVB radiation through the skin during basking. That makes the UVB setup the first place to look when metabolic bone disease is suspected, because a degraded or incorrectly positioned bulb is the most common root cause by a significant margin.
When D3 levels drop, the parathyroid gland responds by pulling calcium directly from bone tissue to keep blood calcium stable. The bone mineral is replaced by fibrous tissue, leaving the skeleton progressively soft and pliable.
Vets call this NSHP, short for nutritional secondary hyperparathyroidism, which is the clinical name for what most keepers know as MBD. Understanding that this disease is the body’s own compensation mechanism, not a sudden illness, helps explain why it develops so slowly and why symptoms appear so late.
Your UVB Bulb Is Probably the Problem
UVB output degrades long before a fluorescent tube burns out. A T8 tube can lose up to 50% of its effective UVB output within six months while still appearing to emit normal light. That gap between visible light and actual UVB is where a large number of metabolic bone disease cases quietly begin, because the keeper sees a glowing tube and assumes the setup is working.
T5 HO tubes hold output better, but most manufacturers still recommend replacement at 12 months regardless of whether the tube still looks fine. Keepers who leave a bulb in for 18 or 24 months because it glows are running a setup that can no longer support adequate D3 synthesis.
The dragon’s body has already started compensating by raiding its own bones. Write the installation date on a piece of tape stuck to your fixture so there is never any ambiguity about when replacement is due.
Distance matters almost as much as bulb age. A T5 HO mounted more than 12 inches from the basking surface delivers sharply reduced UVI output, and a dragon sitting too far below the tube may be absorbing almost no UVB even with a new bulb installed. This is also why coil bulb setups carry greater MBD risk than T5 HO installations, because their UVB field is narrower, degrades faster, and drops off more steeply with distance.
One additional trap that catches keepers by surprise: a correct T5 HO tube sitting on top of a fine mesh screen loses 30–50% of its UV output to the mesh. The tube looks correctly positioned and the right age, but the dragon underneath is receiving a fraction of the UVI it needs.
Mount the fixture inside the enclosure wherever the design allows, or confirm the tube output is strong enough to compensate for the mesh reduction.
One factor that rarely gets mentioned is the relationship between basking temperature and D3 synthesis. D3 production requires the dragon to thermoregulate at the correct temperature while under UVB. A basking spot running too cool on the actual surface can limit D3 synthesis even if the bulb is perfect and fresh.
Confirming basking surface temperature with a digital probe directly on the rock or tile removes the guesswork. Ambient thermometers and stick-on gauges read air temperature, not surface temperature, and they consistently underreport by 10–20°F in a warm enclosure.
The Diet Side Nobody Talks About
UVB gets most of the attention, but dietary calcium failure is equally capable of causing MBD in bearded dragons. The core issue is the calcium-to-phosphorus ratio of the diet. Phosphorus competes directly with calcium absorption in the gut, so a diet heavy in high-phosphorus feeders can drive calcium deficiency even when D3 levels are adequate and UVB is correct.
Most feeder insects have a poor calcium-to-phosphorus ratio and need to be offset by consistent dusting and calcium-rich greens. Crickets are workable with regular dusting, but dragons whose diet skews heavily toward insects and short on leafy greens are at real risk regardless of their lighting setup.
Mealworms are the worst offender. Their Ca:P ratio sits at roughly 1:7, meaning the phosphorus load from a mealworm-heavy diet actively works against calcium absorption. Using mealworms as a staple feeder is a direct route to calcium deficiency regardless of how carefully the rest of the setup is managed.
Gut-loading your feeders before offering them improves the nutritional profile in useful ways, but it cannot correct a bad Ca:P ratio on its own. Gut loading addresses the quality of micronutrients inside the insect. It does not solve the phosphorus competition problem.
You still need to dust, and you still need a diet that is not primarily insect-based in adult dragons.
There is also the D3 oversupplementation risk that most guides ignore. Skin-synthesised D3 is self-regulating, meaning the dragon’s body stops producing it once blood levels are sufficient. Supplemental D3 from powder carries no such mechanism.
If your UVB setup is adequate and you are still dusting with calcium-plus-D3 at every single feed, you risk accumulation. That is why dusting frequency and product choice needs to match how strong your UVB actually is, not just follow a single universal schedule.

The Risk Nobody Warns Egg-Laying Females About
Female bearded dragons will produce and lay unfertilised eggs whether or not they have ever been near a male. The body pulls calcium directly from the skeleton to build eggshells, and that draw is significant.
A female on a perfectly managed setup can slide into acute metabolic bone disease quickly if her calcium intake is not increased substantially in the weeks before and after laying.
This catches keepers off guard because the dragon has been eating well, the UVB is correct, and the dusting schedule has been consistent. None of that is enough during a laying cycle without deliberate supplementation adjustment.
If your female is showing pre-laying behaviour such as restlessness, digging, and appetite changes, increase calcium dusting to daily and monitor her closely for the weeks following the lay.
Bearded Dragon MBD Symptoms to Catch Early
The challenge is that bearded dragons mask weakness well, and the earliest bearded dragon MBD symptoms overlap with several other common problems. A keeper tracking temperature, feeding schedules, and stool consistency can miss the first warnings until something more obvious appears.
The Trembling Most Keepers Mistake for Cold
The very first physical sign in many cases is fine trembling in the forelimbs when the dragon is held or when it tries to push itself off the ground. This is different from the small movements of a dragon settling into your hand.
It is a consistent vibration that persists when the dragon is otherwise relaxed, and it typically starts in the front legs before spreading to the hind limbs as the condition progresses.
A dragon that is reluctant to climb, that stops using elevated hides or branches it previously used with ease, or that spends unusually long periods lying flat on the enclosure floor may be experiencing early-stage muscle weakness linked to calcium loss. The same dragon might also be avoiding the basking spot because moving into position has become physically difficult.
When the Damage Is Already Done
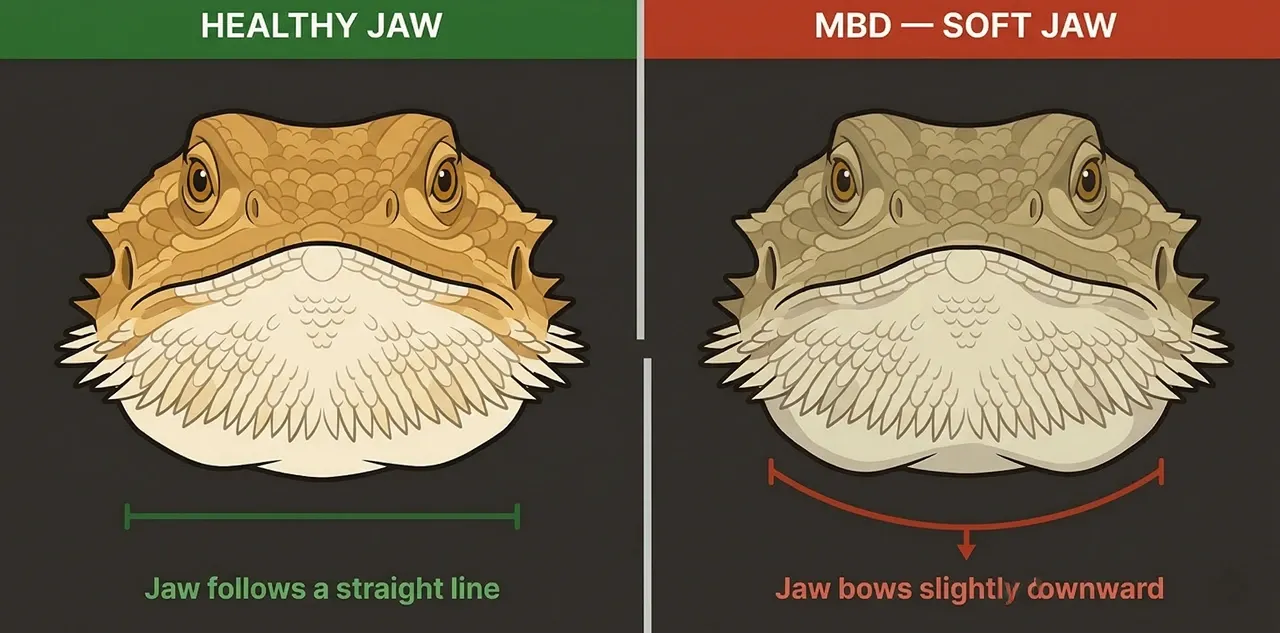
By moderate-stage MBD, the physical changes become hard to miss. The lower jaw starts to feel soft when pressed gently. The facial bones may look subtly swollen.
Hind limb deformity, where one or both back legs bow outward or sit at an unnatural angle during rest, indicates bone that has been demineralising for some time. At this point, the keeper is no longer seeing early signs. The disease is established.
At this stage, the dragon often cannot support its own weight properly. It pancakes flat on the substrate rather than holding a normal upright posture. Spontaneous fractures become a real risk in severe cases, where bones break from ordinary movement with no trauma involved. If your dragon has reached this point, a vet visit is not optional.
How quickly these signs progress depends significantly on age. A juvenile can move from early trembling to visible bone deformity in a matter of weeks, while an adult on a long-term marginal setup may take months to reach the same point. That slower progression in adults is exactly why the early signs get attributed to something else for so long.
| Sign You Are Seeing | Likely Stage | What to Do |
|---|---|---|
| Fine limb trembling when held | Early | Full husbandry audit immediately; vet check if trembling continues after corrections |
| Reduced activity, reluctance to climb | Early | Check UVB age and distance, verify basking surface temp, review diet |
| Soft jaw or slight facial swelling | Moderate | Vet visit required; do not attempt home treatment alone |
| Hind limb bowing or abnormal resting angle | Moderate to severe | Vet visit urgently; X-rays needed to assess bone density |
| Cannot support own weight, pancaking flat | Severe | Vet today; handle with extreme care to avoid fractures |
| Bones breaking without trauma | Severe | Emergency vet; do not attempt to move the dragon unnecessarily |
Dragging Back Legs Is Not Always Impaction
There is a misdiagnosis that costs dragons their lives. When a bearded dragon starts dragging its hind legs, the first conclusion many keepers reach is impaction from sand or substrate. Impaction is real and serious, but hind leg paralysis is the defining symptom of severe MBD, not impaction.
When the spine loses enough calcium, it softens and compresses the nerves running to the hind legs, producing what looks identical to a spinal injury.
The distinction that matters: a dragon with severe impaction will typically stop passing waste entirely. A dragon with spinal MBD may still defecate normally while unable to move its back legs. If your dragon is dragging its legs but still producing waste, check your lighting immediately rather than your substrate.
How to Treat MBD in Bearded Dragons
The honest answer is that it depends entirely on how far the disease has progressed when you catch it. Early-stage MBD, where the only signs are subtle trembling and reduced activity, is frequently reversible with husbandry correction alone.
Replace the UVB bulb, fix the basking distance, improve the diet, correct the dusting protocol, and many dragons show measurable improvement within 4–8 weeks.
Moderate cases, where some bone softening is already visible but no structural deformity has set in, typically need veterinary intervention alongside the husbandry changes. Bone can remineralise with treatment, but the timeline is months rather than weeks. Most dragons recover meaningful function, though mild bowing that has already calcified in a deformed position may remain permanently.
Severe MBD in bearded dragons, where the skeleton has already deformed or fractures have occurred, cannot be fully reversed. The structural changes are permanent. What treatment does in severe cases is stabilise the animal, halt further progression, and improve quality of life. A dragon that was dragging its legs may regain some mobility with proper support and time, but the underlying bone deformity will not resolve.
What a Vet Does That You Cannot
For anything beyond the mildest presentation, this is not a condition you manage at home. A reptile vet will take radiographs to assess actual bone density and check for fractures that may not be visibly obvious.
Blood work covering calcium, phosphorus, and kidney function tells the vet how the body is currently compensating and what the treatment priorities are.
Treatment typically involves injectable calcium gluconate and vitamin D3 to bypass gut absorption and rapidly raise blood levels. In severe cases, calcitonin injections help drive calcium back into bone tissue. Both require prescription and accurate dosing, because overdosing injectable calcium carries cardiac risk. This is not something that can be replicated safely with pet store supplements alone.
Dragons with severe MBD also need supportive care during recovery: careful handling to avoid fractures, a flat enclosure with no climbing structures to fall from, and hand-feeding if jaw weakness makes independent eating difficult. VCA Animal Hospitals also recommends removing all enclosure-mates during recovery to eliminate stress and the risk of contact-related injury.
How to Set Up a Recovery Enclosure
A standard setup with climbing branches and hammocks becomes a fracture risk for a dragon with softened bones. Once MBD is confirmed at moderate stage or above, the enclosure needs to change before anything else.
A dragon with brittle bones can fracture a leg falling three inches from a hammock it has used safely for months.
- Remove all climbing structures. Branches, hammocks, ramps, anything elevated. Everything comes out.
- Lower the basking surface. Flat slate tiles directly on the enclosure floor. Maximum height of any surface is two inches off the ground.
- Reposition your lights. The basking surface is now lower, so your heat lamp and UVB tube need to come down with it. Confirm the floor still reaches 105–115°F and the UVI at basking height is still in the 4.0–6.0 range.
- Switch to paper towel substrate. Easy to change, sterile, and every dropping is visible for monitoring during recovery.
Recovery is slow. Most dragons show improved energy and appetite within one to two weeks of corrected husbandry and vet-prescribed calcium treatment.
Actual bone hardening takes considerably longer. Full re-calcification across a moderate case typically takes three to six months of strict, consistent care. A recovering dragon is also at elevated risk of dehydration during treatment, so weekly warm soaks help support hydration without adding handling stress.
How to Prevent Metabolic Bone Disease in Bearded Dragons
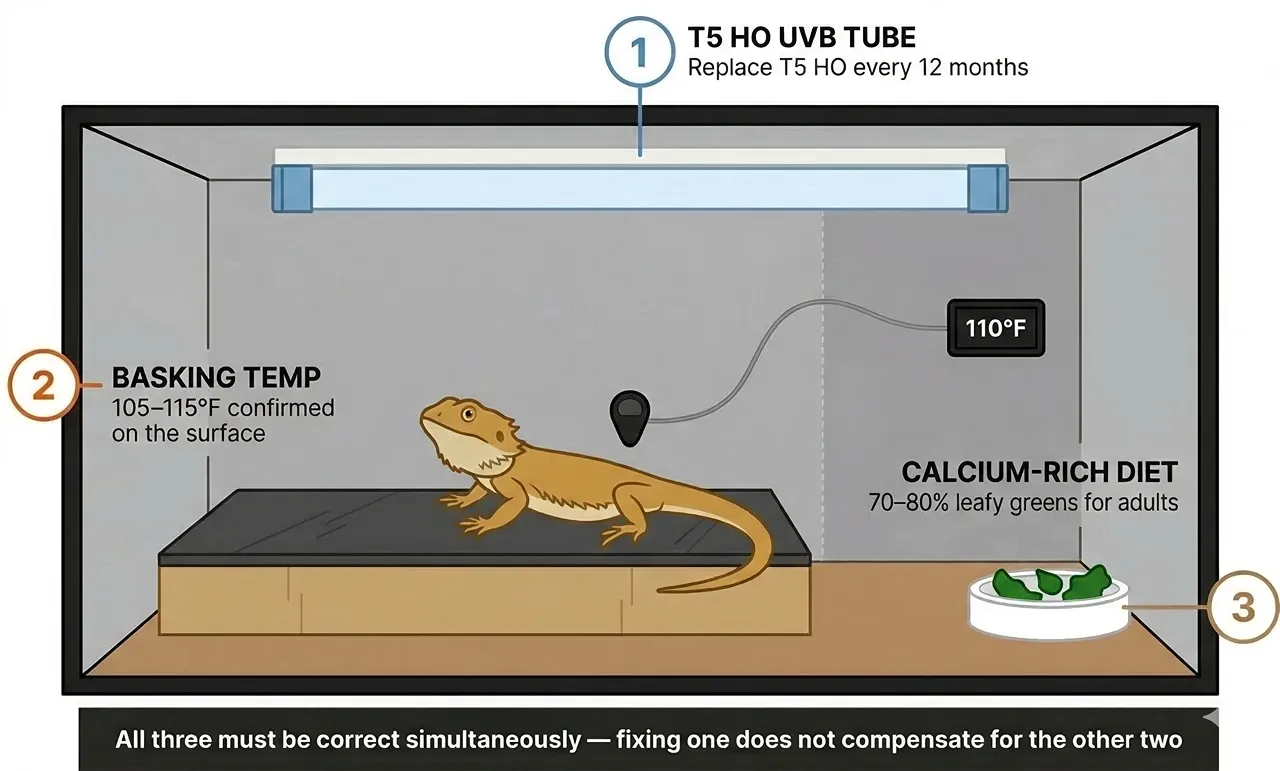
Prevention comes down to three systems running correctly at the same time: UVB quality, basking temperature, and diet. All three need to be in order simultaneously.
A perfect UVB setup does not compensate for a calcium-deficient diet, and a well-dusted diet does not compensate for a failing bulb. MBD in bearded dragons almost always develops at the intersection of two problems, not one.
Replace UVB tubes on a fixed schedule, not based on whether they still look lit. T5 HO tubes at 12 months. T8 tubes at 6 months. Mark the installation date on the fixture with a permanent marker so there is no ambiguity when the next replacement is due.
Basking spot setup is where a large number of preventable cases originate. Dragons need a basking surface temperature of 105–115°F, confirmed with a digital probe or temperature gun directly on the tile, slate, or rock. Air temperature readings will underreport the actual surface heat by a significant margin and should not be used as the reference point for assessing whether D3 synthesis is possible.
On the diet side, adult dragons should be eating 70–80% leafy greens. Collard greens, mustard greens, endive, and turnip greens all carry solid calcium profiles.
Insect feeders remain important for protein, particularly in younger dragons, but they should not dominate an adult’s diet. The dusting schedule needs to account for how much insect protein is being offered relative to the UVB output the dragon is actually receiving.
One risk most guides overlook is brumation. Dragons heading into brumation with any calcium deficit are at elevated risk during dormancy, because they stop eating for weeks or months while their body continues drawing on whatever reserves remain. If anything looked off before your dragon went down, have it checked by a vet before the next feeding season starts.
Getting the full lighting setup right before symptoms appear is far easier than correcting metabolic bone disease once it has taken hold. Tube type, fixture, mounting height, and photoperiod all feed directly into whether your dragon synthesises adequate D3, and errors at any of those points accumulate silently over months before the first visible sign appears.
Knowing what not to do once you spot a problem is just as important as the prevention steps above. The impulse to add more calcium immediately is understandable, but self-treating with high-dose supplements before a vet assessment carries its own risks.
Frequently Asked Questions
How quickly can MBD develop in a bearded dragon
MBD typically develops over weeks to months of consistent UVB or dietary failure. In young, fast-growing juveniles, visible bone demineralisation can appear within 6–8 weeks of inadequate UVB exposure. Adults develop it more slowly, which is also why cases in older dragons tend to be more advanced before they are caught.
Is metabolic bone disease painful for bearded dragons
Yes. Soft bones and micro-fractures cause ongoing discomfort that is easy to miss because dragons do not vocalise pain. A dragon that has always been calm to handle and suddenly becomes defensive when picked up may be reacting to pain rather than a temperament shift. That change in handling behaviour is worth taking seriously as a symptom in its own right.
Should I use calcium with D3 or without
Both, but not on the same schedule. Calcium without D3 goes on feeders four to five times per week. Calcium with D3 or a reptile multivitamin once per week. Most D3 should come from a correctly set up UVB source. Over-supplementing dietary D3 risks hypercalcemia, where calcium deposits form in organ tissue, which is genuinely dangerous and the reason D3 powder should never be used daily.
Can a bearded dragon live normally after MBD
Many dragons with mild to moderate MBD make strong functional recoveries once the husbandry is corrected and veterinary treatment is completed. Permanent bone deformity, particularly in the hind limbs, is possible but does not necessarily prevent a good quality of life. Severe structural damage with ongoing fracture risk requires continued veterinary assessment rather than a single treatment course.
At what age are bearded dragons most at risk
Juveniles under 18 months are at the highest risk because their bones are actively growing and the demand for calcium and D3 is at its peak. Husbandry errors that a healthy adult tolerates for months will affect a fast-growing juvenile far more quickly. That said, adults on long-term inadequate setups are far from immune.
Fix the Setup Now, Not After the Next Symptom
- Check the UVB bulb installation date. A failed bulb is the single most common driver of MBD in bearded dragons that goes undetected for months. If you cannot remember when it was installed, treat it as overdue and replace it. T5 HO tubes at 12 months. T8 tubes at 6 months. Write the date on the fixture.
- Check whether your fixture sits above mesh. If the tube is outside the enclosure on top of a screen lid, assume 30–50% UVI loss. Either mount the tube inside or upgrade to a more powerful output tube that compensates for the reduction.
- Verify basking surface temperature with a digital probe or temperature gun directly on the tile, slate, or rock. Target 105–115°F. Do not use an ambient thermometer or stick-on gauge as your reference point.
- Audit your dusting protocol. Confirm the dusting frequency matches your dragon’s age and that you are not using calcium-plus-D3 at every single feed if your UVB output is adequate.
- Review the diet. Adults should be 70–80% leafy greens. If mealworms are a regular staple, remove them. Crickets, dubia roaches, and black soldier fly larvae offer a far better Ca:P ratio.
- If any symptoms are already present, including trembling limbs, soft jaw, reluctance to climb, or abnormal posture, book a vet appointment now. Do not wait to see whether the husbandry corrections alone will fix it.
Medical Disclaimer: This article is written for educational purposes and reflects general husbandry experience. It is not a substitute for professional veterinary advice. If your bearded dragon is showing any symptoms of illness or injury, contact a reptile-experienced veterinarian. Early professional assessment makes a significant difference in outcomes for health conditions like MBD.

Written by
Sarah ArdleySarah has kept bearded dragons for over ten years. She founded Beardie Husbandry after discovering that most mainstream care advice — including what she followed with her first dragon — was doing more harm than good. Every article on this site is grounded in veterinary research and real keeper experience.