Bearded Dragon Mouth Rot (Stomatitis): Early Signs, Gentle Care, and Prevention
That yellowish film along the gum line is not leftover food and it is not a shedding artefact. Bearded dragon mouth rot is one of the few reptile health conditions that shows up visually before the dragon even stops eating.
That gives you a real window to act before things spiral.
Caught at stage one, most cases resolve with an appropriate antibiotic course prescribed by a reptile vet. Left untreated, the bacteria migrate into the jawbone, and at that point the situation becomes considerably more complicated and far slower to resolve.
What Mouth Rot Actually Is
Infectious stomatitis is the medical term for bearded dragon mouth rot. It is a bacterial infection of the oral tissues, most commonly driven by opportunistic gram-negative bacteria including Aeromonas, Pseudomonas, and Fusobacterium. These bacteria live in the environment and on the skin normally.
The problem begins when oral tissue is compromised and the immune system cannot keep bacterial populations in check. An injury, a temperature dip, or a dirty enclosure provides the conditions; the bacteria do the rest.
One thing that consistently surprises owners is the type of discharge involved. Reptiles do not produce liquid pus the way mammals do.
Instead, infected tissue creates a dry, chalky, cottage-cheese-like material called caseous exudate. If you see this substance in your dragon’s mouth, that is infected tissue, not food residue and not shed material.
Bearded dragon mouth rot is less common in this species than in iguanas or water dragons, but it occurs often enough that every keeper needs to know the early signs. Poor husbandry creates the conditions; a small injury or immune dip gives the bacteria their opening.
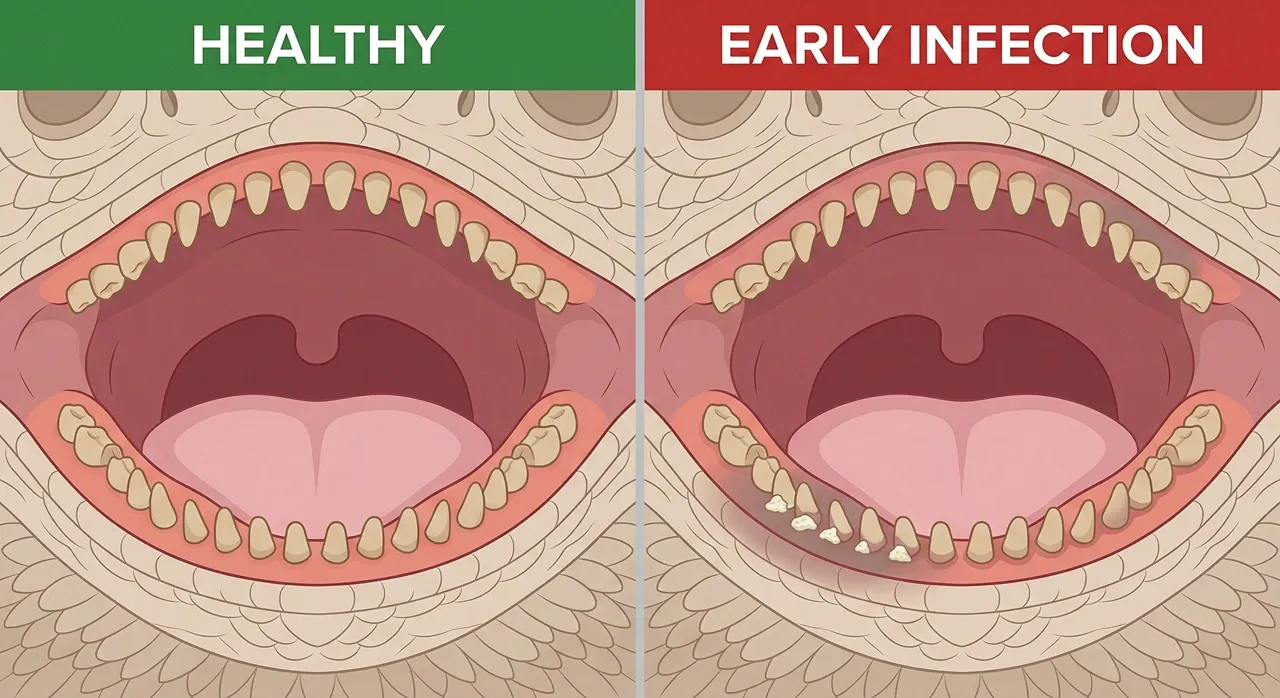
Early Signs That Are Easy to Miss
The problem with catching it early is that bearded dragons do not broadcast discomfort. A keeper who checks the enclosure from the outside and ticks feeding and basking off the list can miss the first signs for weeks. Getting hands on the animal and actually opening the mouth regularly matters.
The Gum Colour Shift
Healthy gum tissue in a bearded dragon is a consistent pink throughout the oral cavity. When stomatitis begins, the tissue shifts to a dusky red or grey first, then to a mottled, inflamed appearance concentrated around one patch.
This is usually most visible along the lower jaw where the gum meets the tooth row.
The change is subtle at stage one, but it is there. Bright redness in one concentrated area, rather than uniform pink across the whole mouth, warrants a closer look and a call to the vet.
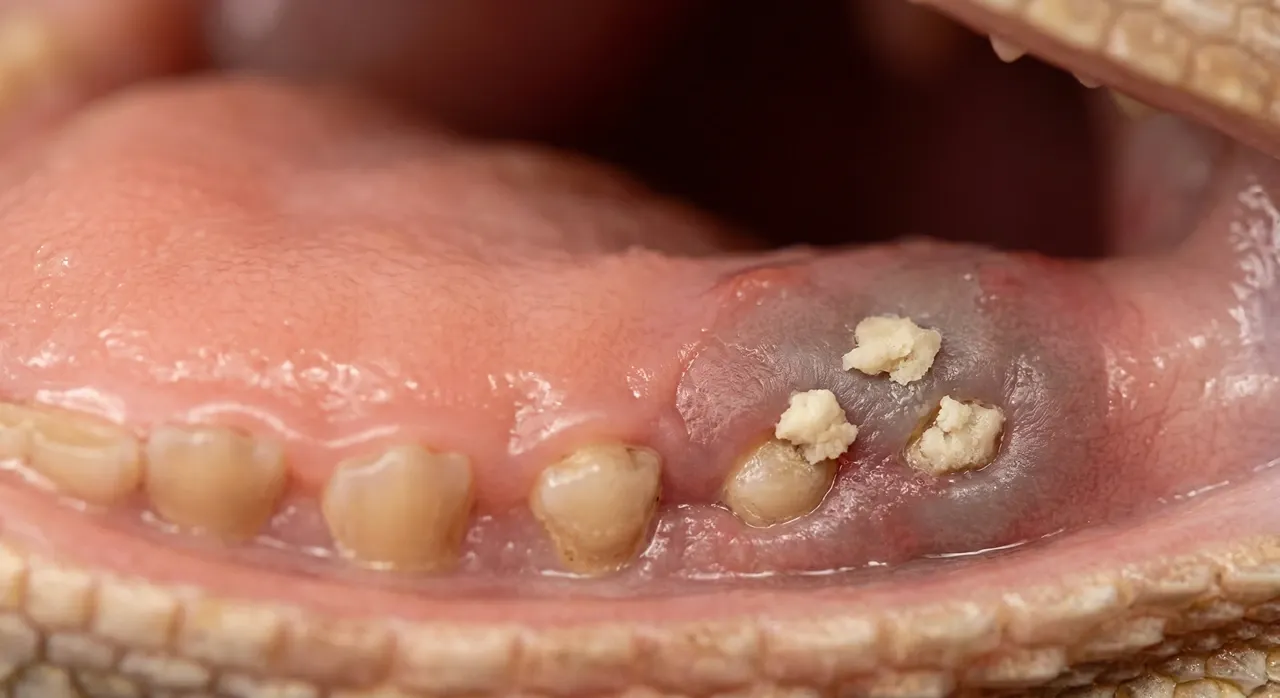
That Caseous Discharge
Before the infection becomes obvious, small deposits of white or yellowish material start forming at the gum margins or around the base of teeth. This is the caseous exudate unique to reptile infections: dry, crumbly, and slightly adherent to the tissue beneath it.
It does not wipe away cleanly the way food does, and it tends to reappear within a day of being removed.
A single small deposit does not automatically confirm mouth rot, but it warrants monitoring and a vet conversation that same week. Do not attempt to scrape it away forcibly. That damages tissue that is already inflamed and can drive bacteria deeper into the wound.
Going Quiet and Off Food
One of the subtler early signs of bearded dragon mouth rot is a behavioural shift before visible oral changes appear. A dragon in the early stages of stomatitis often becomes slightly less engaged, and handling sessions that used to be relaxed become squirmy.
The appetite dips, but not dramatically enough to trigger alarm on its own.
If your dragon is eating less than normal and you notice any change to mouth colour or texture, treat those two signals together rather than separately. Individually, both are easy to explain away. Together, they are a reason to open the mouth and look carefully under a proper light source.
⚠ Skip Home Monitoring and Call a Vet Today If You See Any of These
Total refusal to eat or drink. Visible jaw swelling from the outside. Caseous material spreading rapidly across multiple areas. Discharge from the nostrils or eyes. Any of these signals means the infection has already progressed past the earliest stage. The window for simple treatment is closing.
Signs the Infection Is Spreading
Stage one stomatitis stays localised to a small patch of oral tissue. When treatment does not come quickly enough, bacteria move through the oral cavity and into surrounding structures. The signs at this stage are harder to miss, but the situation is also considerably harder to treat.
Jaw Swelling Visible From the Outside
Visible swelling along the jaw line, particularly on one side, suggests the infection has reached deeper tissue or bone. This is a same-day veterinary concern.
Jaw swelling from bearded dragon mouth rot should never be attributed to mating behaviour or a large recent meal until a vet has confirmed it is not infectious.
Thick Stringy Saliva
Healthy bearded dragons produce very little visible saliva. When stomatitis progresses, the saliva becomes thick, rope-like, and sometimes discoloured grey, yellow, or faintly bloody. You may notice the dragon struggling to close its mouth fully, or strings of abnormal saliva stretching between the jaw and tongue when it opens.
A dragon that refuses to drink due to oral pain deteriorates quickly. Dehydration signs like skin tenting and sunken eyes can develop within days once a beardie stops taking in fluids.
Discharge from the Nose or Eyes
When the infection reaches this stage, it has moved well beyond the oral cavity. Nasal or eye discharge alongside visible oral disease suggests systemic bacterial involvement. This is a veterinary emergency, not a situation for continued home monitoring.
Discharge from the nares alongside lethargy can also overlap with a respiratory infection, which sometimes develops concurrently when the immune system is already under pressure from oral disease. A vet needs to assess which condition is primary before prescribing treatment.
What Actually Causes Mouth Rot in Bearded Dragons
Bacteria are the mechanism, but they are rarely the root cause on their own. Something in the dragon’s environment or body creates the opening that allows a normal oral bacterial population to become the kind of infection that drives bearded dragon mouth rot.
There are three main contributors, and most cases involve more than one.
Husbandry Failures Set the Stage
Suboptimal temperatures are the biggest underlying factor in most cases of stomatitis. A beardie living on a basking surface of 95°F rather than 105–110°F has a measurably impaired immune response.
That immune dip does not cause bearded dragon mouth rot directly, but it leaves the oral tissue far less capable of managing bacterial populations that a healthy animal would clear without issue.
Sustained high humidity is a contributing factor, particularly in enclosures running above 50% consistently. Excess moisture encourages bacterial growth on surfaces the dragon contacts with its face and mouth every day.
A dirty enclosure amplifies this further. Encrusted feeders left overnight, uncleared substrate, and decor with biofilm buildup all increase the bacterial load the oral tissue is exposed to on a daily basis.
Cricket Bites and Physical Injuries
This is the cause that most articles mention briefly then pass over, but it deserves proper attention because it is extremely common.
Crickets left in the enclosure overnight will bite. A sleeping beardie is a soft target, and a bite to the lip margin or gum line is a direct entry point for bacteria into tissue that would otherwise be intact.
The same logic applies to abrasions from nose-rubbing against the glass. Glass surfing produces repeated micro-abrasions on the lips and snout that introduce bacteria directly into tissue over time.
Any time your dragon sustains a visible oral injury from a cricket bite, a misaimed feeding, or snout abrasion, monitor the area daily for three to five days for localised redness or early caseous material.

Low Basking Temps and Immune Suppression
Bearded dragons are ectotherms. Their immune function is temperature-dependent in a way that mammal owners sometimes underestimate. A dragon that cannot reach an adequate basking surface temperature of 105–110°F does not mount a normal immune response. That is a physiological impairment, not just a comfort issue.
Calcium and vitamin D3 deficiencies also suppress immune competence over time. A dragon on a poorly maintained calcium and D3 schedule becomes progressively more vulnerable to opportunistic infections that a nutritionally sound animal would resist without difficulty.
How a Vet Diagnoses and Treats It
A reptile vet examines the oral cavity directly and assesses the extent of tissue involvement. Where the infection appears to involve deeper structures, X-rays confirm whether the jawbone has been affected.
A bacterial culture identifies the exact pathogen, which matters considerably when selecting an antibiotic, since prescribing the wrong drug risks treatment failure and contributes to resistance.
| Severity | What You See | Typical Vet Treatment |
|---|---|---|
| Stage 1 (Early) | Mild gum redness, small caseous deposits, slight appetite dip | Oral antibiotics, antiseptic mouth rinse, husbandry correction review |
| Stage 2 (Moderate) | Spreading caseous material, swollen gums, significant appetite loss | Injectable antibiotics, antiseptic flushing at the clinic, possible tissue debridement |
| Stage 3 (Severe) | External jaw swelling, tooth loosening or loss, nasal or eye discharge | Injectable antibiotics, surgical removal of necrotic tissue, X-ray to assess bone, assisted feeding |
Over-the-counter fish antibiotics are not a safe substitute for a prescription. The correct drug type, dose, and duration depend on the specific pathogen and the dragon’s body weight.
A course that uses the wrong antibiotic leaves resistant bacteria behind. They re-establish faster than the original infection, and the second round is harder to clear than the first.
According to VCA Animal Hospitals, infectious stomatitis typically requires injectable antibiotics as well as antiseptic mouth rinses, with supplemental feeding needed for dragons too painful to eat on their own.

What to Do While Waiting for the Vet
The vet appointment is the priority. These steps support the dragon and stop the environment from actively making things worse while you wait. They are not a replacement for professional treatment.
💡 Home Support While Awaiting Vet Care
Remove all feeders immediately. No crickets, no roaches, nothing live in the enclosure until the infection has cleared. A cricket bite right now is the last thing this dragon needs.
Disinfect the enclosure thoroughly. Clean all surfaces, decor, the basking area, and the food dish. Reduce the bacterial load in the environment as much as possible before the vet appointment.
Verify basking surface temperature with a temp gun. Not an adhesive strip. Use a laser infrared thermometer directly on the spot the dragon sits. If it is not hitting 105–110°F, fix it immediately.
Offer soft, finely chopped foods. Collard greens, butternut squash, thinly sliced bell pepper. Foods that require minimal jaw pressure keep nutrition going without forcing the dragon to work an infected mouth.
Do not scrape the caseous material yourself unless a vet has specifically guided you through the correct dilution and technique. Aggressive home cleaning of infected oral tissue can drive bacteria into deeper layers or cause bleeding that worsens the infection.
Mouth Rot or Yellow Fungus
These two conditions are sometimes confused in early stages because both can produce visible abnormalities around the face and mouth. Telling them apart matters because the treatment approach differs entirely: antifungals for yellow fungus, antibiotics for stomatitis. Using the wrong treatment wastes time the dragon does not have.
| Feature | Mouth Rot (Stomatitis) | Yellow Fungus (CANV) |
|---|---|---|
| Primary location | Inside the oral cavity: gums, teeth, tongue | Often on skin and scales; may enter the mouth secondarily |
| Discharge type | Caseous (dry, cottage-cheese-like) inside the mouth | Yellow-brown thickened plaques on the skin surface |
| Spread pattern | Tracks from oral tissue into jaw and bone | Aggressively invades through scale and muscle |
| Smell | Foul bacterial odour from the mouth | Often no significant odour in early stages |
| Treatment | Prescription antibiotics; good prognosis if caught early | Antifungals (voriconazole); prognosis often guarded to poor |
If the lesions are on the outside of the face or lips rather than the oral tissue itself, or if scales around the face appear thickened, discoloured, or flaking, yellow fungus disease needs to be ruled out.
A vet culture swab is the only reliable way to confirm which condition you are dealing with before treatment begins.
How Long Recovery Takes
Bearded dragon mouth rot at stage one, treated promptly with the correct antibiotic, typically shows improvement within seven to ten days. The caseous material reduces, gum colour returns towards normal, and appetite comes back.
The full antibiotic course usually runs two to four weeks. Stopping early because the dragon looks better is one of the most common mistakes. Residual bacteria re-establish faster than the original population, and the second round is harder to clear.
Stage two cases take four to six weeks, with vet rechecks confirming the infection is clearing rather than just suppressed. Jawbone involvement at stage three means months of treatment, possible repeat debridement, and no guarantee of full recovery.
During recovery, softer foods keep nutrition up without forcing the dragon to use a sore mouth. Finely chopped leafy greens from the safe foods list hold moisture and require minimal jaw pressure. Hard-shelled insects stay off the menu until the vet confirms the oral tissue has healed.
Preventing Mouth Rot Long-Term
Remove Live Feeders After Every Session
Never leave live crickets in the enclosure overnight. A hungry cricket will bite anything warm, and a sleeping beardie is a prime target. Feed live insects during the day, watch the session, and pull any uneaten feeders before the lights go off.
Keep Basking Temperatures Correct
An immune-competent beardie resists opportunistic bacterial infection far more effectively than one living below optimal temperature. Validate your basking surface regularly with a laser infrared thermometer directly on the spot the dragon sits.
The surface needs to hit 105–110°F, not the air above it. Ambient readings consistently understate surface temperature by several degrees, so always use a direct surface measurement rather than an air probe or adhesive strip.
Maintain a Clean Enclosure
Spot-clean daily. Do a full disinfect of decor and surfaces monthly, or more often if the dragon defecates regularly in one area. Biofilm on rocks and wood is invisible to the eye but meaningfully increases bacterial exposure for an animal that investigates everything with its tongue and snout.
Keeping decor sanitised also reduces the risk that intestinal parasites take hold. Parasites add immune load that makes bacterial infections harder to fight off.
Support Immune Function Through Diet
A nutritionally complete diet with correct calcium dusting and D3 supplementation keeps the immune system working as it should. Dragons on a monotonous feeder insect rotation with no leafy green variety become progressively more vulnerable.
That kind of immune dip makes bearded dragon mouth rot far more likely to establish in tissue that a well-nourished animal would clear on its own.
A supplement schedule that has quietly drifted out of routine has the same effect. Consistent dusting is not optional when it comes to keeping a beardie’s defences working properly.

Frequently Asked Questions
Can You Treat Mouth Rot at Home
Not effectively. Bearded dragon mouth rot requires prescription antibiotics to clear. Antiseptic rinses can slow progression while you arrange an appointment, but they will not eliminate the bacterial infection. Attempting to treat without a confirmed diagnosis and appropriate medication risks the infection advancing to the jawbone.
What Does Mouth Rot Smell Like
A foul, sour-to-rotten odour coming from the mouth is a consistent sign. Bearded dragons do not normally produce any noticeable breath smell, so any persistent unpleasant odour, especially combined with visible tissue changes, warrants a close look and a vet call.
Can a Dirty Bowl Cause Mouth Rot
A biofilm-coated water bowl increases bacterial exposure, but bearded dragon mouth rot typically requires a tissue entry point for bacteria to establish an infection. A wound, abrasion, or immune compromise is usually the deciding factor.
That said, keep water dishes and food bowls clean regardless, as they contribute to overall enclosure pathogen load.
Can mouth rot make your dragon lose teeth
In moderate to severe cases of bearded dragon mouth rot, yes. The infection causes gum recession and dental loosening as it progresses through oral tissue. Bearded dragon teeth do not regenerate, so any tooth loss from stomatitis is permanent. Early treatment is the only way to prevent this outcome.
Can mouth rot come back after treatment
Yes, if the underlying husbandry issue that allowed the infection to take hold has not been fixed. A dragon that recovered from stomatitis in a too-cool or too-dirty enclosure is at real risk of recurrence.
Use the follow-up vet appointment to review the setup thoroughly, not just the dragon’s oral health.
What to Check Right Now
If something in your dragon’s mouth does not look right, the clearest next step is a thorough look inside and a call to a reptile vet. Open the mouth gently under a proper light source and check against all five of these.
- Pink, uniform gum tissue across the full oral cavity with no red patches, grey areas, or puffiness
- No white or yellow deposits at the gum margin or between teeth
- No unpleasant smell when the mouth is open
- Clear, thin saliva with no stringiness, discolouration, or excessive production
- No swelling visible along the jaw line when viewed from the outside
A healthy beardie passes all five without any question. Anything that falls short is a reason to call a reptile vet today. Bearded dragon mouth rot moves faster than most owners realise, and the early stage is the only one that keeps treatment simple, affordable, and effective.
Medical Disclaimer: The information in this article is intended for educational purposes only and does not constitute veterinary advice. If you suspect your bearded dragon has mouth rot or any other health condition, consult a qualified reptile veterinarian promptly for an accurate diagnosis and appropriate treatment plan.

Written by
Sarah ArdleySarah has kept bearded dragons for over ten years. She founded Beardie Husbandry after discovering that most mainstream care advice — including what she followed with her first dragon — was doing more harm than good. Every article on this site is grounded in veterinary research and real keeper experience.







